molecular and translational allergoloGy
The Molecular and Translational Allergology (MTA) team focuses on patient-centered research aiming to address and solve unmet medical needs in allergy diagnosis and prevention.
Background
Allergic diseases are steadily on the rise and while being considered as nuisance disorder over the past decades, they represent now the most common chronic disease in Europe. Beyond the individual disease burden for each patient, substantial socioeconomic costs result from allergic conditions which can be measured, amongst others, by the reduced quality of life of patients and their families, reduced productivity, as well as in-/direct costs for medical care. Currently, more than 150 million Europeans suffer from an allergic disease and the prevalence is still increasing.
Allergy bears on a multifaceted pathophysiology with patients showing a broad spectrum of clinical pictures, including variable clinical symptoms, levels of clinical reactivity, atopic comorbidities and disease progression. The complexity of the factors involved explains why diagnostic and therapeutic measures still pose a challenge and thus, represent important unmet medical needs.
To unravel the pathophysiological basis and immune mechanism of allergic sensitisation as well as clinical allergy, it is vital to develop translational approaches for diagnosis, treatment and prevention of allergies – the latter being clearly a major long-term goal.
Mission
The Molecular and Translational Allergology (MTA) team focuses on patient-centered research aiming to address and solve unmet medical needs in allergy diagnosis and prevention. The research is performed in close collaboration with other teams at the Department of Infection and Immunity, other LIH departments and technological platforms, as well as with leading clinical and scientific experts at the Centre Hospitalier de Luxembourg, University of Luxembourg, Luxembourg Institute of Science and Technology and a number of clinical and research excellence centers in Europe.
Activities
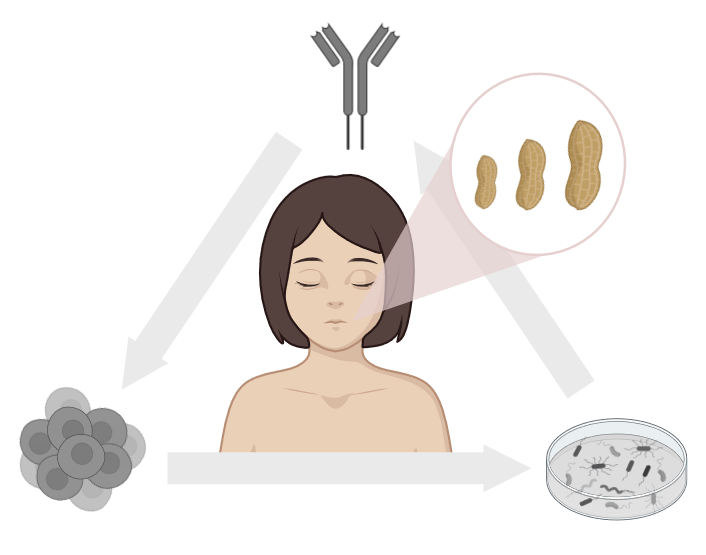
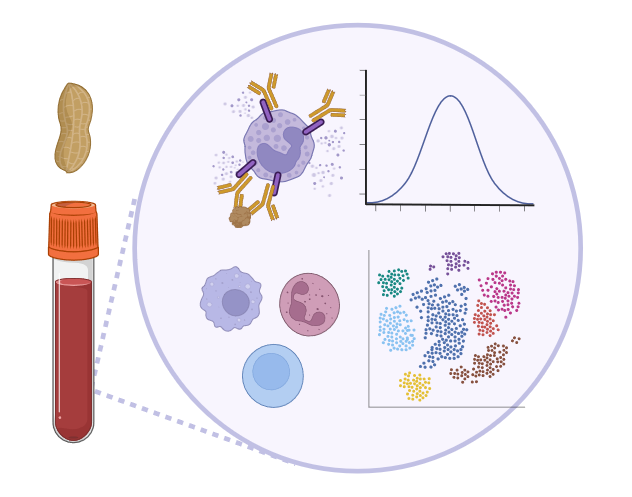
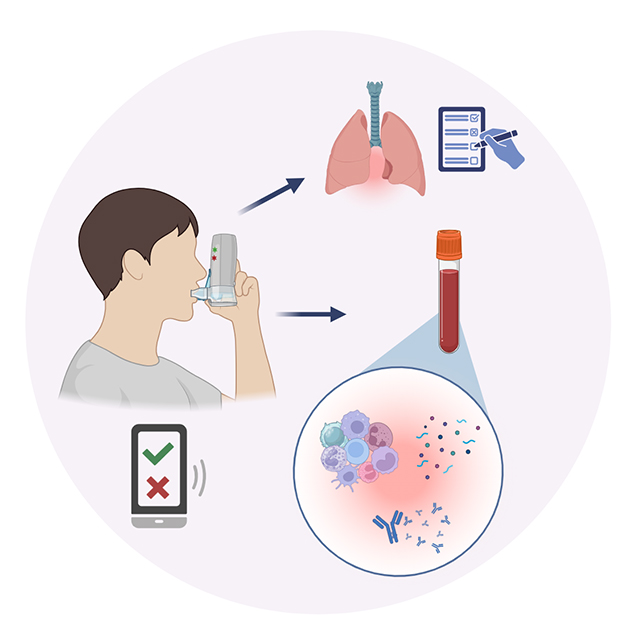
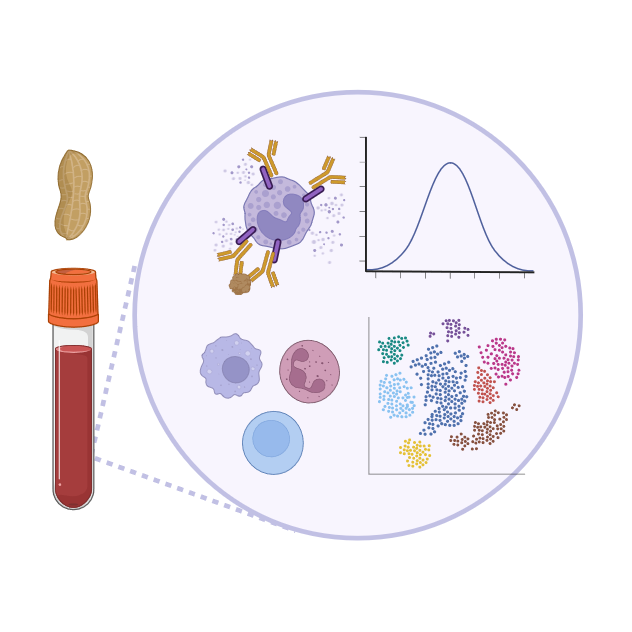
Our research focuses on: i) allergen molecules, which are key players, both as sensitisers and triggers in allergic reactions; ii) biomarkers identifying early pathological immune reactions to naturally occurring and otherwise harmless substances in air and food. Allergen-based insights and deep immunophenotyping address important aspects of the complex multifactorial puzzle.
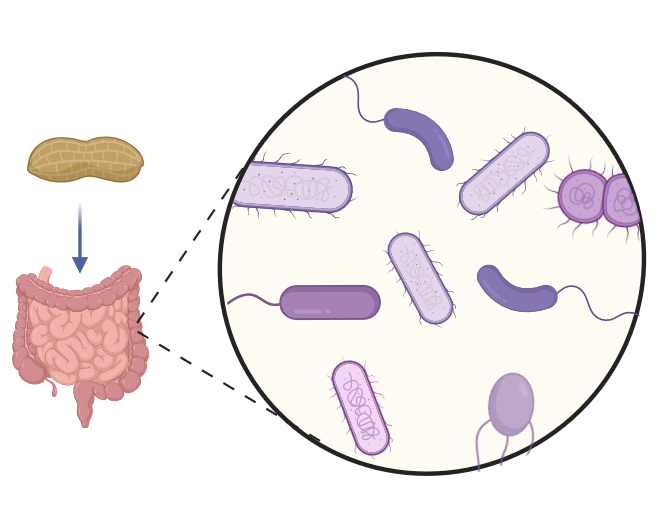
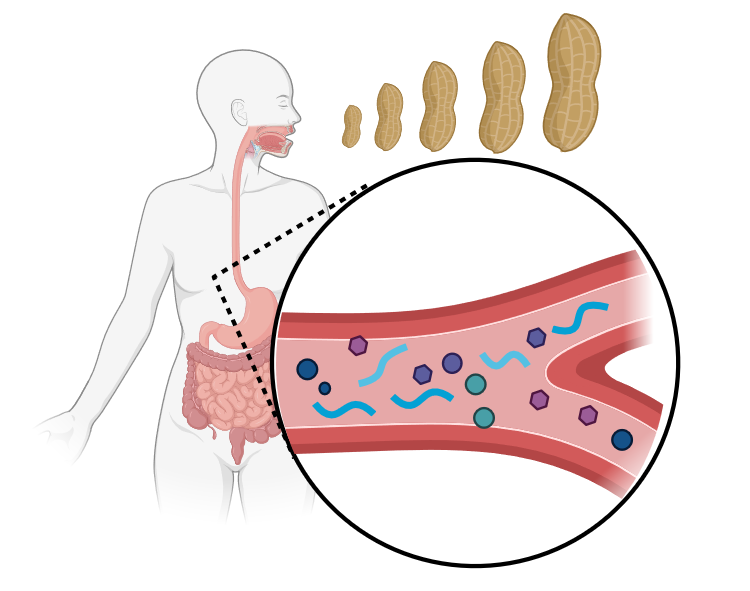
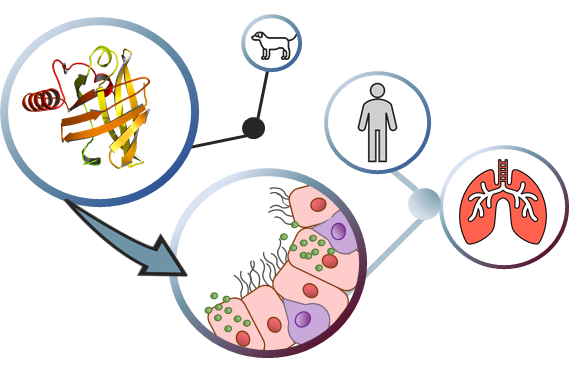
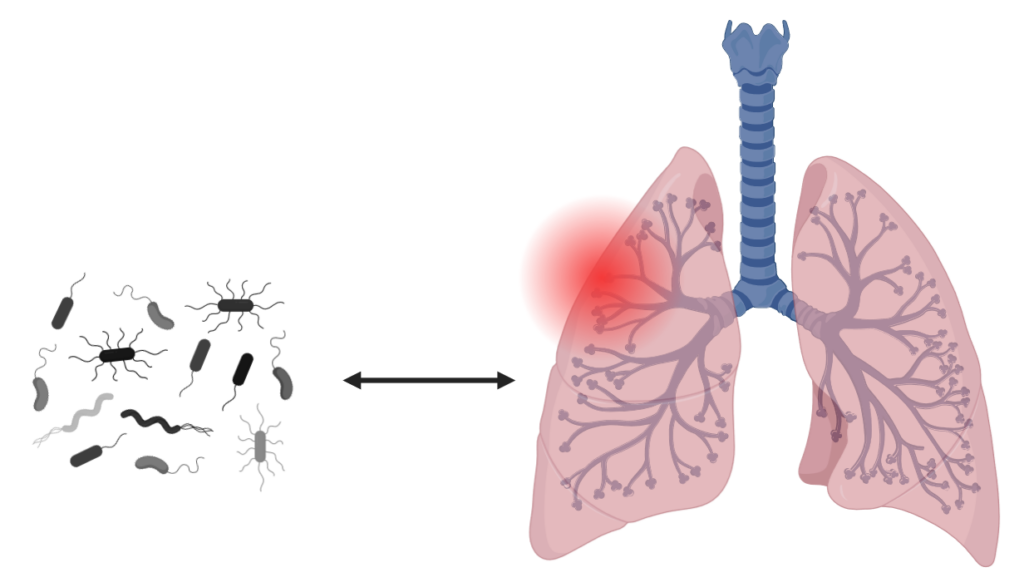
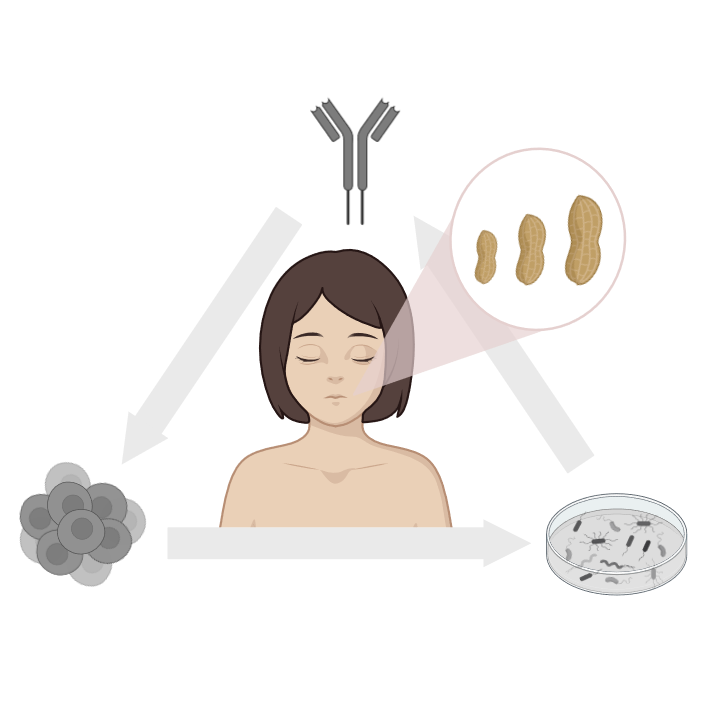
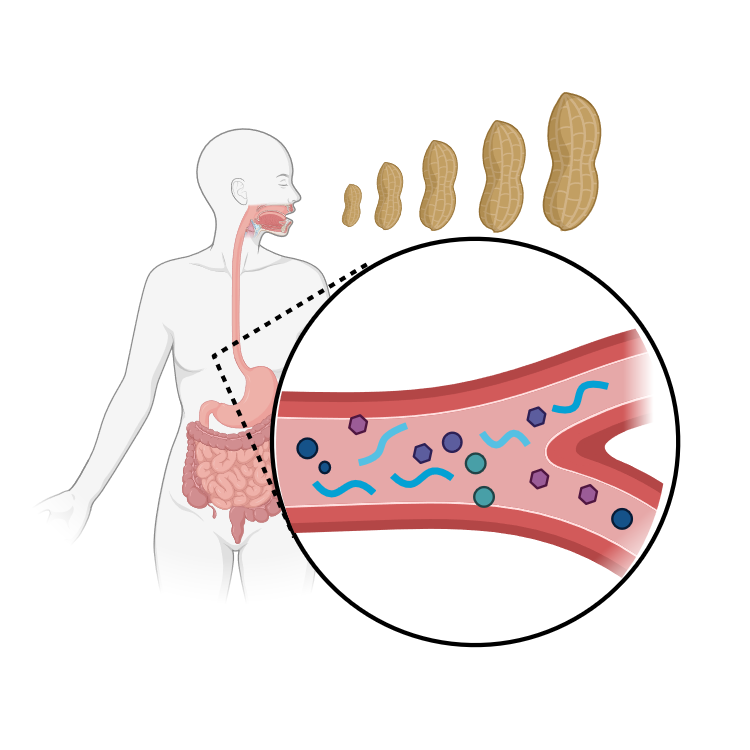
The knowledge around allergens, their molecular and immunological properties, helps to address mechanisms of allergic sensitisation and anaphylaxis, by understanding how allergens enter the human body, cross mucosal epithelia and impact the host microbiome, how they interact with the immune system in order to finally identify advanced biomarkers applicable for the stratification of allergic patients. Inflammatory processes and break of tolerance are the starting points of many allergic diseases manifesting as allergic rhinitis, asthma, atopic dermatitis or food allergy. Unravelling the underlying pathophysiological immune mechanisms of break of tolerance and understanding early life priming of the immune system will ultimately lead to the development of prevention and treatment strategies for allergic diseases.
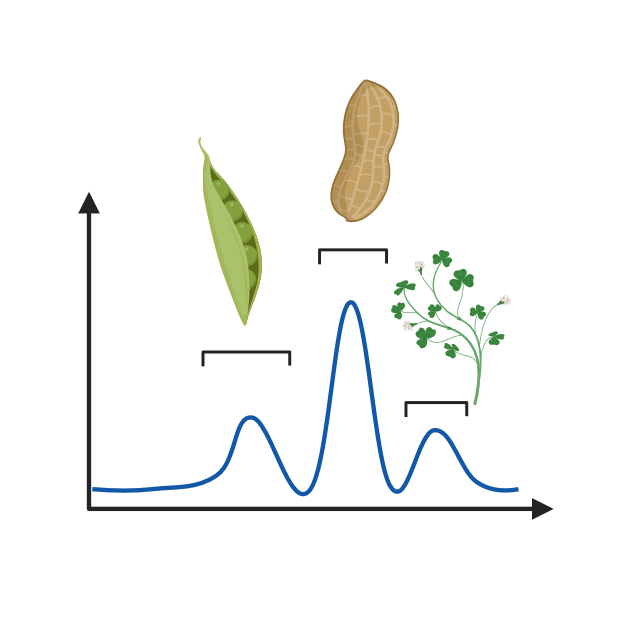
Today, the use of single allergens in serum IgE-testing allows deeper insights into the disease cause and course, such as to discriminate between genuine sensitisation and cross-reactivity, as well as to identify potentially mild from severe allergy phenotypes. In addition to serum IgE-typing, the development of new immune biomarkers will allow to identify the patients’ molecular profile and potential responders to available immunotherapies, an important step towards personalised treatment.
We are closely linked to the clinical practice through our partner, the National Service of Immuno-Allergology at CHL, as well as to a number of clinical and research excellence centers in Europe.
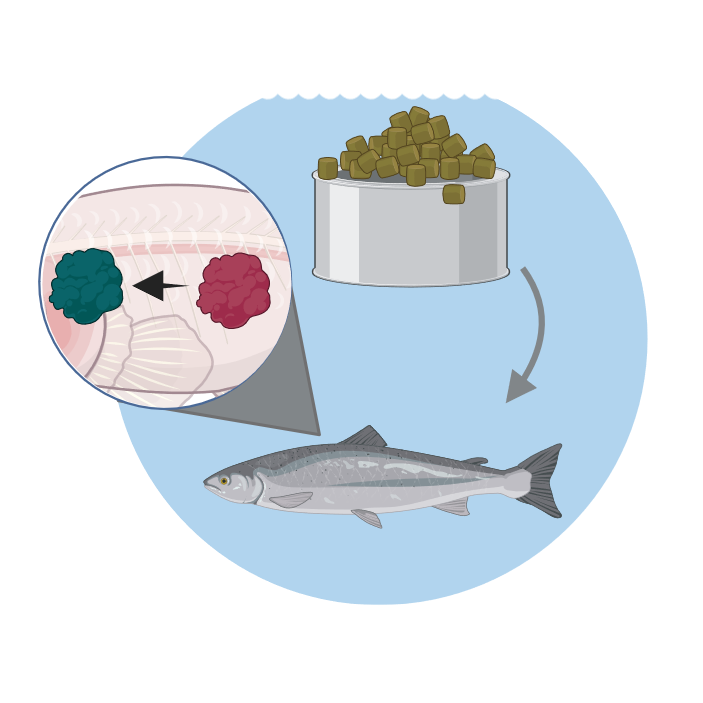
Clinical relevance of allergens
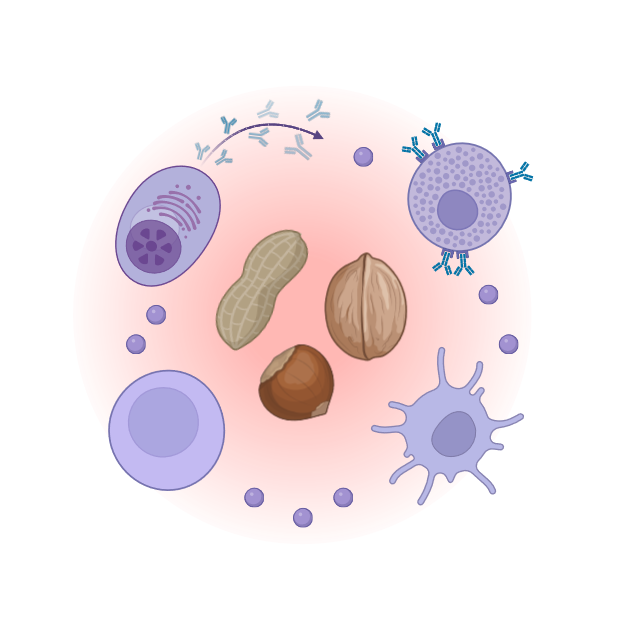
Immune responses underlying food allergy
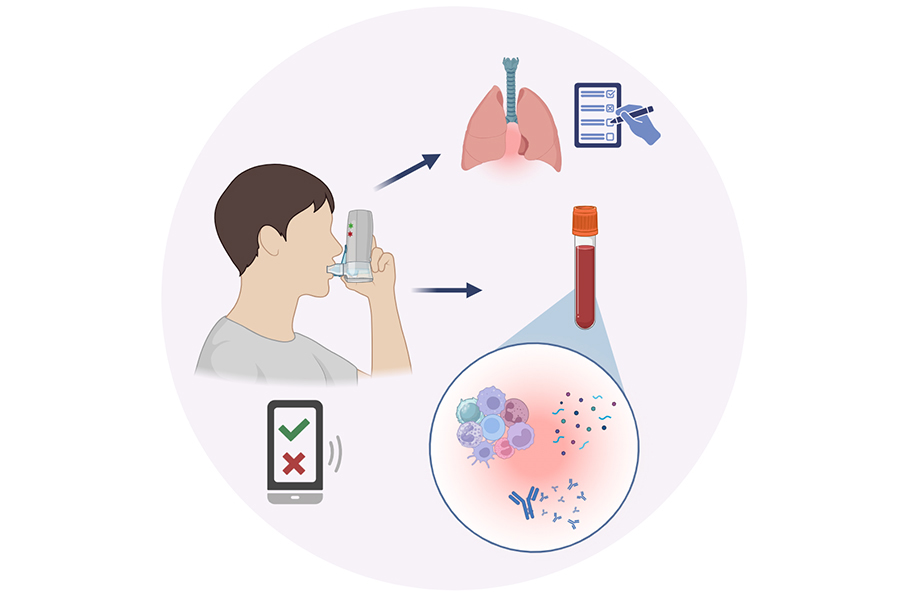
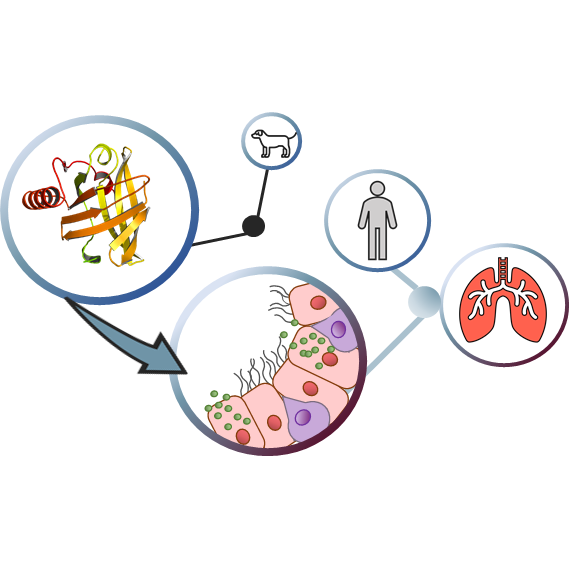
Immune responses underlying respiratory allergy
Transversal research projects
Funding Support
Partners
Projects & clinical trials
Featured team members
Scientific publications
-
Assessing the Allergenic Relevance of Vespula alascensis Venom – 20/11/2025
-
Algorithms in Allergy – 26/01/2026
-
Sequence of Immunological Events During IgE-Mediated Allergic Reactions to Food – 24/12/2025
-
Combined exposure to shrimp tropomyosin and microbial components triggers enhanced allergic and inflammatory responses in vitro – 24/11/2025
-
Birch rust allergy as a novel autumnal trigger of seasonal airway symptoms – 06/11/2025
-
Co-occurrence of memory impairment and fatigue distinguishes post COVID from pandemic-related health effects in the 4-year CON-VINCE cohort study – 27/10/2025
-
Oral Immunotherapy of Peanut Allergy – 01/08/2025
-
The Use of Omics Sciences in Allergic Diseases From Bench to Bedside – 02/07/2025
-
Fecal IgE Analyses Reveal a Role for Stratifying Peanut-Allergic Patients – 26/07/2024
-
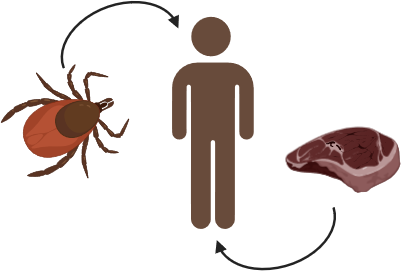
Longitudinal Follow-up Reveals Peripheral Immunological Changes Upon Tick Bite in α-Gal–Sensitized Individuals – 29/07/2025
Related News

Job vacancies
There are no jobs matching this page at the moment. You can view all jobs via the button below.